5 results
A tale of excess: the curious case of the woman with 1447 emergency visits
- M. Sagué Vilavella, A. Giménez Palomo, A. Àvila-Parcet, T. Fernández Plaza, L. Navarro Cortés, G. Oretega Hernández, M. Pons Cabrera, L. Tardón Senabre, M. Vázquez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S286
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Frequent attenders to emergency services are challenging and costly. We report the case of a woman in her mid-twenties who stands out for a total of 1447 emergency visits.
ObjectivesOur primary objective was to describe the emergency visits of our patient. Secondary objectives were to assess her use of other healthcare services and to calculate her health expenditure.
MethodsThis is a clinical case report. We reviewed the patient’s electronic medical records for sociodemographic and clinical data. We obtained detailed information of psychiatric ED visits (length, most frequent times and days) regarding the second most-visited hospital. We assessed the efficacy of hospitalizations in reducing ED visits with a paired samples t Test, comparing the number of visits 30 days pre- and post-hospitalization. We estimated the health expenditure using the regional public health system prices, including three direct costs: emergency visits, hospitalizations and ambulance transportation. We obtained written informed consent from the patient’s legal guardian.
ResultsA 26-year-old woman from Barcelona (Catalonia, Spain), diagnosed with mild intellectual disability, made 1447 emergency visits between 2009 and 2021 (figure 1). 946 visits (65%) took place in psychiatric emergency departments (EDs), whilst 353 (24%) in non-psychiatric EDs and 148 (10%) in urgent primary care. She attended 24 hospitals (ranking number one the closest to the patient’s home, with 387 visits) and seven primary care centers, distributed across 17 cities in Catalonia. Most visits were self-referred, being the main presenting problems anxiety and instrumental suicidal behaviour. Saturday was her favorite day for hospital visits (24,1%), while she seeked care on Tuesdays much less often (4.5%). She made 73.5% of consultations between 1pm and 6pm, with a median length per visit of 2.8 hours (range 0.33-20.9 hours). Regarding other therapeutic approaches, she attended day hospitals, psychiatric rehabilitation programs and family therapy, among others (figure 2), for which she showed low adherence and scarce benefit. She had ten acute hospitalizations, interventions that did not reduce ED visits (t=-0.9835, p=0.36). Health expenditure reached 410.035€.
Image:
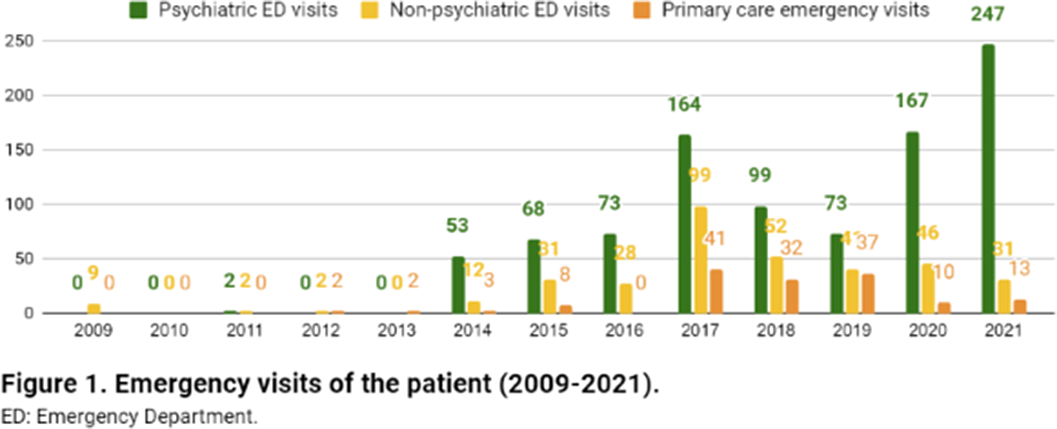
Image 2:
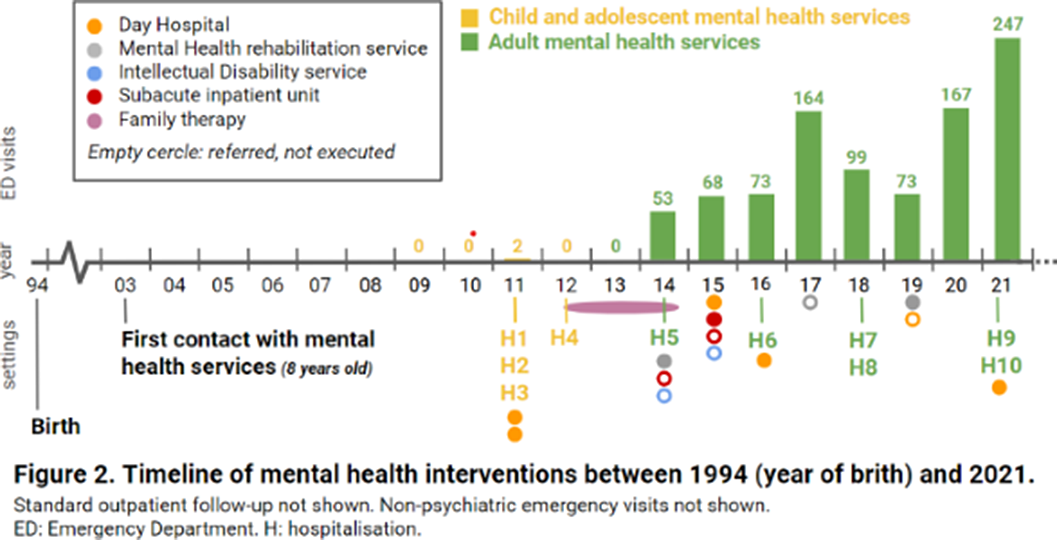 Conclusions
ConclusionsThe most common definition of frequent attendance is a patient who has five or more visits per year. Many times, but not always, repeat visits are also inappropriate. The case we report is a grotesque example of both frequent and inappropriate attendance, which has been resistant to all kinds of interventions and has quality-of-care, financial and ethical implications. As of today, it is still a pending case. Maybe it is worth considering residential treatment?
Disclosure of InterestNone Declared
Double dystonia secondary to risperidone: acute laryngeal dystonia and oculogyric crisis.
- L. Tardon, O. Marco, L. Navarro, T. Fernandez, O. de Juan, M. Bioque, H. Andreu
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S1066
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Acute laryngeal dystonia due to antipsychotics is an uncommon but potentially lethal form of extrapyramidal reaction. The initial symptoms may be subtle but progressively appear difficulties in phonation, stridor and dyspnea which are often life-threatening.
ObjectivesTo describe a case of acute laryngeal dystonia and oculogyric crisis secondary to risperidone.
MethodsThe present study is a case report of a patient admitted for schizophrenia who was presented a laryngeal dystonia and oculogyric crisis after being treated with 5mg risperidone. We also searched previously case reports, series and systematic reviews of laryngeal dystonia using a pubmed query.
ResultsA 30-year-old Caucasian woman who was admitted for schizophrenia presented rhinolalia, oropharynx paresthesias, mild dyspnea without stridor, and prolonged involuntary upword desviation of the eyes. All these symptoms started within 24 hours of starting risperidone 5mg per day. A laryngoscopy showed abnormal motion of the vocal cords that suggested laryngeal dystonia. Symptoms remitted after administration of intramuscular biperiden 4mg. Risperidone was later switched to olanzapine because of better psychomotor side-effect profile.
ConclusionsLaryngeal dystonia is a medical emergency requiring early diagnosis and immediate treatment. Anticholinergic agents should be carried out, without waiting for the results of complementary tests. The route of administration can be intramuscular or intravenous. This complication should be always kept into account when a patient is taking any antipsychotic, and remembered for the antipsychotic election in following treatments.
Disclosure of InterestNone Declared
Anticholinergic syndrome in a patient with schizophrenia
- O. Marco Estrada, L. Tardon, T. Fernández, L. Navarro, M. Bioque, N. Arbelo
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S790
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Anticholinergic syndrome (AS) is a complication that can appear due to different drugs with antimuscarinic effects, such as antihistamines, alkaloids, antipsychotics, tricyclic antidepressives or anesthetics, and it is characterized by urinary retention, dry mouth and skin, mydriasis, low-grade fever, and confusion or coma.
ObjectivesTo describe a clinical case of AS admitted to our hospital.
MethodsWe present a case report of a patient with schizophrenia who presented an anticholinergic syndrome. We also searched for previous studies of AS using a pubmed query.
ResultsA 53-year-old male was admitted for a psychotic decompensation to another hospital in Barcelona. The usual treatment at home was amisulpride 1200mg/d, olanzapine 30mg/d and lormetazepam, and haloperidol 6mg/d and clotiapine 40mg/d were added to treat the decompensation. Then, the patient started to present mydriasis, mucocutaneous dryness, low-grade fever, slight hypertension and tachycardia, repeated retentions of urine, confusion, unintelligible speech and agitation, so he was referred to our hospital. Once he was admitted, haloperidol was withdrawn and support measures (bladder catheterization, fluid therapy, etc.) were applied. After a few days, most of the mentioned alterations were stabilized, but the psychotic symptoms, such as thought and behavioural disorganization, persisted and required electroconvulsive therapy, with subsequent improvement.
ConclusionsAS is a relatively frequent side effect of psychiatric medication, which diagnosis is clinical, so, we must be capable to identify it and initiate early treatment to prevent possible complications. The first step, as reflected in the case described, is to stop the causative drugs, and apply support measures. Additionally, physostigmine can be used, as it is an effective antidote.
DisclosureNo significant relationships.
Trichotillomania in adulthood, a case report
- L. Navarro, T. Fernández, L. Tardon, O. Marco, N. Arbelo, N. Baldaquí, M. Cavero
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S177
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Trichotillomania is a disorder (estimated prevalence 0.5-2.0%) with common onset in childhood, rarely seen in adulthood, characterized by the repetitive pulling out of one’s own hair leading to hair loss and functional impairment, associated with other comorbidities: major depression (39-65%), anxiety disorder (23-32%), SUDs (15-19%), OCD (13-27%).
ObjectivesTo present a case of late-onset trichotillomania in a 60-year-old woman.
MethodsThe present study is a case report of a patient visited in outpatient psychiatry for trichotillomania. We also searched previously case reports, series and systematic reviews of clinical trichotillomania using a pubmed query.
ResultsThis is a 60-year-old morbidly obese woman diagnosed with dysthymia, binge eating disorder and histrionic personality disorder. She explained a worsening of anxiety associated with work problems of one year of evolution and, for six months, the beginning of the plucking of eyebrow hairs and scabs to decrease this symptom, with inability to avoid the behaviour and without eating the hairs. The mental evaluation highlighted psychic anxiety, hypothymia, low self-esteem and feelings of failure and did not suggest a delirium. We started treatment with topiramate up to 150mg/day which was not successful. After that we switched to fluoxetine up to 60mg/day associated to psychotherapy observing a slight gradual improvement.
ConclusionsThe clinical presentation suggested the diagnosis of trichotillomania in the context of dysthymia. No particular medication demonstrates efficacy in the treatment of trichotillomania. Preliminary evidence suggests treatment effects of clomipramine, NAC and olanzapine based on individual trials with small sample sizes. Research findings also recommend psychotherapy based on habit reversal.
DisclosureNo significant relationships.
Lurasidone-induced mania: A case report
- T. Fernández, L. Navarro, O. Marco, L. Tardon, N. Arbelo, L. Ilzarbe, P. Barrio, I. Pacchiarotti
-
- Journal:
- European Psychiatry / Volume 65 / Issue S1 / June 2022
- Published online by Cambridge University Press:
- 01 September 2022, p. S404
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Lurasidone is an atypical antipsychotic agent with potential antidepressant effects through its antagonist activity at the 5-HT7 receptor. Although treatment-emergent affective switch (TEAS) induced by second-generation antipsychotics are not frequent, several cases have been reported. To our knowledge, there is no evidence of lurasidone-induced TEAS.
ObjectivesTo describe a case of lurasidone-induced mania.
MethodsWe describe a clinical case of a patient admitted to our psychiatric outpatient unit who developed a manic episode, presumably induced by the introduction of lurasidone. We also conduct a review of the literature on this subject.
ResultsA 37-year-old man diagnosed with obsessive-compulsive disorder (OCD) and an alcohol use disorder was hospitalized due to OCD decompensation with depressive symptomatology and suicidal thoughts, and for alcohol detoxification process. Since he had a previous history of clomipramine-induced TEAS, he was started on lurasidone up to 111mg to avoid the use of antidepressants, showing a progressive improvement of depressive symptoms. Thus, the patient was discharged when alcohol detoxification process was completed. Eight days after discharge, the patient began to show manic symptoms, so he had to be readmitted. Lurasidone was discontinued and valproic acid up to 1000mg/day as mood stabilizer was added, presenting a positive remission of manic symptoms.
ConclusionsAccording to our experience, lurasidone may have induced an affective switch in this patient. Based on our findings, patients and psychiatrists should monitor possible lurasidone-induced mood switching. However, further research is needed in order to back-up this one case report findings.
DisclosureNo significant relationships.





